Is Your Immune System Affecting Implantation?
Understanding Recurrent Implantation Failure Through the Lens of Reproductive Immunology
When Everything Looks Right… But Embryo Transfers Still Fail
“Embryos were good quality. Transfer was smooth. The lining was optimal. Yet the result was negative. Again.”
If you have experienced repeated implantation failure (RIF), you know this emotional exhaustion. Each IVF cycle brings hope — and when it fails despite “everything looking normal,” the question becomes harder:
What are we missing?
For many years, implantation was a black box in reproductive medicine. Once the embryo was transferred, we waited. If pregnancy did not occur, explanations were often limited to embryo quality or chance.
But research over the last decade, especially in reproductive immunology and endometrial biology, has shown something important:
Implantation is not just about placing an embryo inside the uterus. It is a highly regulated immune process.
At Horizon Women and Fertility (HWF), we approach repeated implantation failure not as a mystery, but as a clinical pattern that deserves structured evaluation — without overtesting or overpromising.
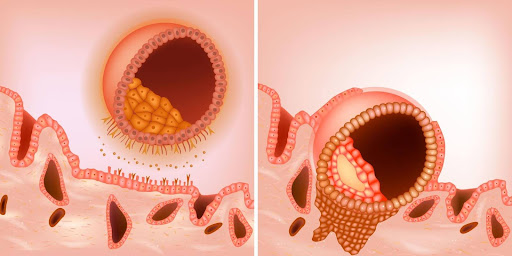
Implantation Is Not Passive — It Is a Biological Dialogue
An embryo is genetically half foreign to a woman’s body. From an immune perspective, it carries paternal genetic material.
So why doesn’t the immune system reject it?
Because implantation is not about suppression it is about controlled immune tolerance.
The uterus creates a temporary, finely tuned inflammatory window. A small, regulated inflammatory response helps the embryo attach and invade. Too little immune activity — implantation fails. Too much — it may be disturbed.
This delicate balance is what reproductive immunology is trying to understand.
When Do We Start Thinking About Immune Factors?
Not every failed IVF cycle needs immune testing. In fact, most do not.
We consider deeper evaluation when there are clear clinical triggers, such as:
- Recurrent implantation failure (typically defined as ≥3 failed transfers of good-quality embryos)
- Recurrent miscarriage
- Repeated failure despite good-grade blastocysts
- History of autoimmune disorders (thyroid disease, lupus, antiphospholipid syndrome)
- Abnormal endometrial biopsy findings
Immune testing should be driven by pattern recognition — not anxiety
What Could Be Happening Beneath the Surface?
Stronger clinical links include:
One of the most important treatable causes
Diagnosis:
1. Uterine Natural Killer (uNK) Cells
These are specialized immune cells present naturally in the uterus. Despite their name, they are not “dangerous killers.”
Their role:
- Help in placental development
- Support blood vessel remodeling
- Regulate early implantation
In some cases, altered activation or imbalance may affect implantation. However, evidence is still evolving. Elevated NK cell levels alone do not automatically mean infertility.
Interpretation requires context.
2. Cytokine Balance (Inflammatory Signals)
The immune system communicates through chemical messengers called cytokines.
Implantation requires:
- Controlled inflammation
- Balanced Th1/Th2 immune response
Excessive pro-inflammatory dominance may disrupt implantation. But again, laboratory numbers alone do not tell the full story.
3. Autoimmune Associations
Certain autoimmune conditions have stronger evidence linking them to implantation problems:
- Thyroid antibodies
- Antiphospholipid syndrome (APS)
- Positive ANA in selected cases
For example:
- Uncontrolled thyroid dysfunction can reduce implantation rates.
- APS is clearly associated with miscarriage and requires anticoagulation treatment.
These are are clinically actionable findings.
4. Chronic Endometritis
This is one of the most important and treatable causes.
Chronic endometritis is low-grade inflammation of the uterine lining. It may not cause symptoms.
Diagnosis:
- Endometrial biopsy
- CD138 plasma cell staining
Multiple recent reproductive studies show improved implantation rates after proper antibiotic treatment in confirmed cases.
Should Everyone Undergoing IVF Get Immune Testing?
Many immune therapies are controversial or still under investigation. Over-testing can create confusion and unnecessary treatment.
At HWF, we do not use immune testing as a routine IVF add-on. It is considered only when:
- Clinical history supports it
- Other common causes are ruled out
- Treatment decisions will change based on results
If Immune Factors Are Identified, What Are the Treatment Options?
Treatment depends entirely on the diagnosis.
Strong Evidence-Based Interventions
- Treat chronic endometritis with antibiotics
- Correct thyroid dysfunction
- Manage antiphospholipid syndrome with anticoagulation (e.g., low molecular weight heparin + low-dose aspirin)
These interventions are supported by established reproductive guidelines.

Moderate or Controversial Therapies
- Low-dose steroids
- Intralipid infusions
- IVIG therapy
Evidence for these remains mixed. They are not universal solutions and must be individualized.
The goal is not to “suppress immunity blindly.”
The goal is to restore balance — only when imbalance is proven.
Maternal Age and Immune Function
Age influences immune behavior.
As maternal age increases:
- Endometrial receptivity changes
- Inflammatory regulation may shift
- Embryo quality declines
Implantation failure is often multifactorial. Immunology is one piece of a larger puzzle — not the only piece.
The HWF Clinical Approach
At Horizon Women and Fertility, our approach to repeated implantation failure is structured and balanced:
- We analyze embryo quality and genetic factors.
- We assess uterine anatomy and endometrial health.
- We optimize hormonal and metabolic status.
- Immune evaluation is considered selectively, not routinely.
- We avoid unnecessary add-ons.
If repeated implantation failure has become part of your journey, a detailed and thoughtful evaluation may help uncover hidden factors — and equally important, avoid unnecessary interventions.
FAQ’S
-
It usually refers to failure of implantation after three transfers of good-quality embryos, though definitions vary slightly across clinics.
Final Thoughts
Recurrent implantation failure can feel isolating and confusing — especially when reports say “everything is normal.”
But implantation is not a simple event. It is a biological conversation between embryo and uterus, regulated by hormones, genetics, blood supply — and yes, the immune system.
What was once a black box is slowly becoming clearer through research.
The key is not aggressive testing.
The key is structured, evidence-aware evaluation.
If you are facing repeated implantation failure, consult with a team that looks beyond routine protocols and approaches your case with clinical depth and care.
At HWF, we are equipped to handle complex implantation challenges — thoughtfully, responsibly, and with your long-term reproductive health in mind.


