From Microbiome to Motherhood: Can “Good Bacteria” Influence Fertility?

Understanding When everything looks right… but pregnancy still doesn’t happen
“All reports are normal.”
“Embryo quality is good.”
“Transfer went smoothly.”
And still, the result is negative.
This is where most couples feel stuck. Not because something is clearly wrong but because nothing seems wrong. In recent years, we’ve started looking at a quieter factor, the microbiome in fertility and uterine health. The body, including the uterus, is not completely sterile. There are bacteria living there, and in some women, this balance may influence implantation success and IVF outcomes.
In such cases, consulting an experienced fertility specialist at a best gynecological clinic can help identify hidden factors.
What exactly is this microbiome?
Simply put, it is the collection of bacteria living in the body.
In fertility, the environment of these two areas matter:
• The vagina, where we already know good bacteria are important
• The uterus, where research is still evolving
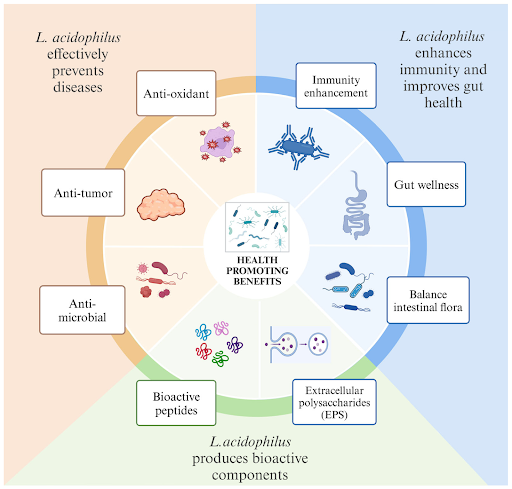
A lower healthy reproductive tract is usually dominated by a group of bacteria called Lactobacillus, considered protective and essential for female fertility health.
Why are these “good bacteria” important?
Lactobacillus helps maintain a slightly acidic environment, which naturally prevents harmful bacteria from growing. It also keeps inflammation low.
Some recent studies have shown that women with a Lactobacillus-dominant microbiome tend to have better implantation rates and improved IVF success, especially when guided by a fertility doctor.
What happens when this balance is disturbed?
This condition is called microbiome dysbiosis, a silent imbalance in the uterus.
There may be no symptoms:
- No pain
- No discharge
It is usually detected through:
- Endometrial biopsy
- CD138 testing (chronic endometritis marker)
In some patients, this can affect implantation or lead to repeated failures. Along with microbiome imbalance, we also see a few common gynecological conditions that quietly affect the uterine environment.
Chronic endometritis is one of them. It is a low-grade, persistent inflammation inside the uterus, often without symptoms. In some women, it is linked to prior events like incomplete miscarriage (RPOC), repeated curettage or evacuation procedures, or unresolved mild infections. If not identified, it can affect implantation and sometimes lead to repeated failures.
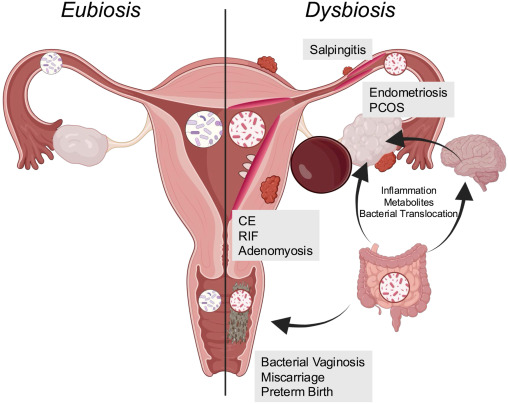
At the vaginal level, symptoms like persistent discharge with fishy odour may suggest bacterial imbalance (like bacterial vaginosis), while thick white discharge with itching is more typical of candidal infection. These are usually treatable, but if neglected, bacteria can ascend upwards in some cases, increasing the risk of uterine or even tubal infection, which over time may contribute to adhesions or tubal damage.
There is also some clinical association between chronic inflammation and endometrial polyps so Hysteroscopy can sometimes help.
Another issue is low Lactobacillus levels
When protective bacteria reduce:
- Other bacteria may grow
- The environment becomes less stable
- Implantation may be affected
Current evidence suggests a pattern:
- Better outcomes when Lactobacillus is dominant
Lower success rates when inflammation is present
Do all patients need microbiome testing?
Most patients do not need microbiome testing. We usually think about it only in situations like:
- Repeated IVF failure
- Recurrent implantation failure
- Unexplained miscarriages
Tests may include:
- Endometrial biopsy
- CD138 staining for chronic endometritis
- Vaginal swabs
-
Advanced microbiome tests for repeated implantation failures and repeatedly positive infection detected in biopsies.
A qualified fertility doctor in a best gynecological clinic will guide the need for testing.
Can this be treated or improved?
Often once detected, treatment is usually straightforward- course of antibiotics.
-
A course of targeted antibiotics is given
-
Followed by probiotics, to restore balance
This is usually done before planning the next embryo transfer.
If there is a focus of infection or lifestyle factor such as uncontrolled diabetis, controlling it helps in avoiding recurrence.
Simple Indian diet changes that help
Daily food habits also help in maintaining a healthy gut and reproductive tract microbiome.
Some practical options:
- Curd (dahi) – simple, effective natural probiotic
- Buttermilk (chaas) – supports digestion and gut balance
- Idli / dosa batter – naturally fermented, good for gut bacteria
- Homemade fermented foods (in moderation)
- Kanji (in some regions)
These support the gut microbiome, which indirectly influences overall inflammation and hormonal balance.
Also include:
- Fruits like banana
- Garlic and onions
- Whole grains like millets and oats
These act as prebiotics—they feed the good bacteria
Lifestyle matters more than people realise
- Avoid unnecessary antibiotics
- Don’t overuse vaginal washes or douching
- Maintain a healthy weight
- Manage stress
These small things quietly affect the internal environment
One important point—many patients try to “self-clean” using vaginal washes or douching. This actually disturbs the natural protective bacteria and can worsen the imbalance.
Summary:
Microbiome is not the main cause in most fertility cases. It is one layer—relevant in some patients, not all. The focus should always be: right test, right patient, right timing.
How we approach this at HWF
For individuals facing repeated IVF failure, unexplained implantation issues, or recurrent miscarriages, a focused and expert approach becomes essential.
At Horizon Women Fertility (HWF), Hyderabad, care is centered on detailed evaluation and personalized treatment—considering factors like uterine health, embryo quality, and microbiome balance when needed.
Under the guidance of Dr. Lavanya Bommakanti, Fertility Specialist & Gynecologist with 15+ years of experience, patients receive thoughtful, evidence-based care tailored to their condition.
The right direction often begins with the right diagnosis by an experienced fertility specialist.


